Mechanical Ventilation: What You Need to Know Before Making This Critical Decision
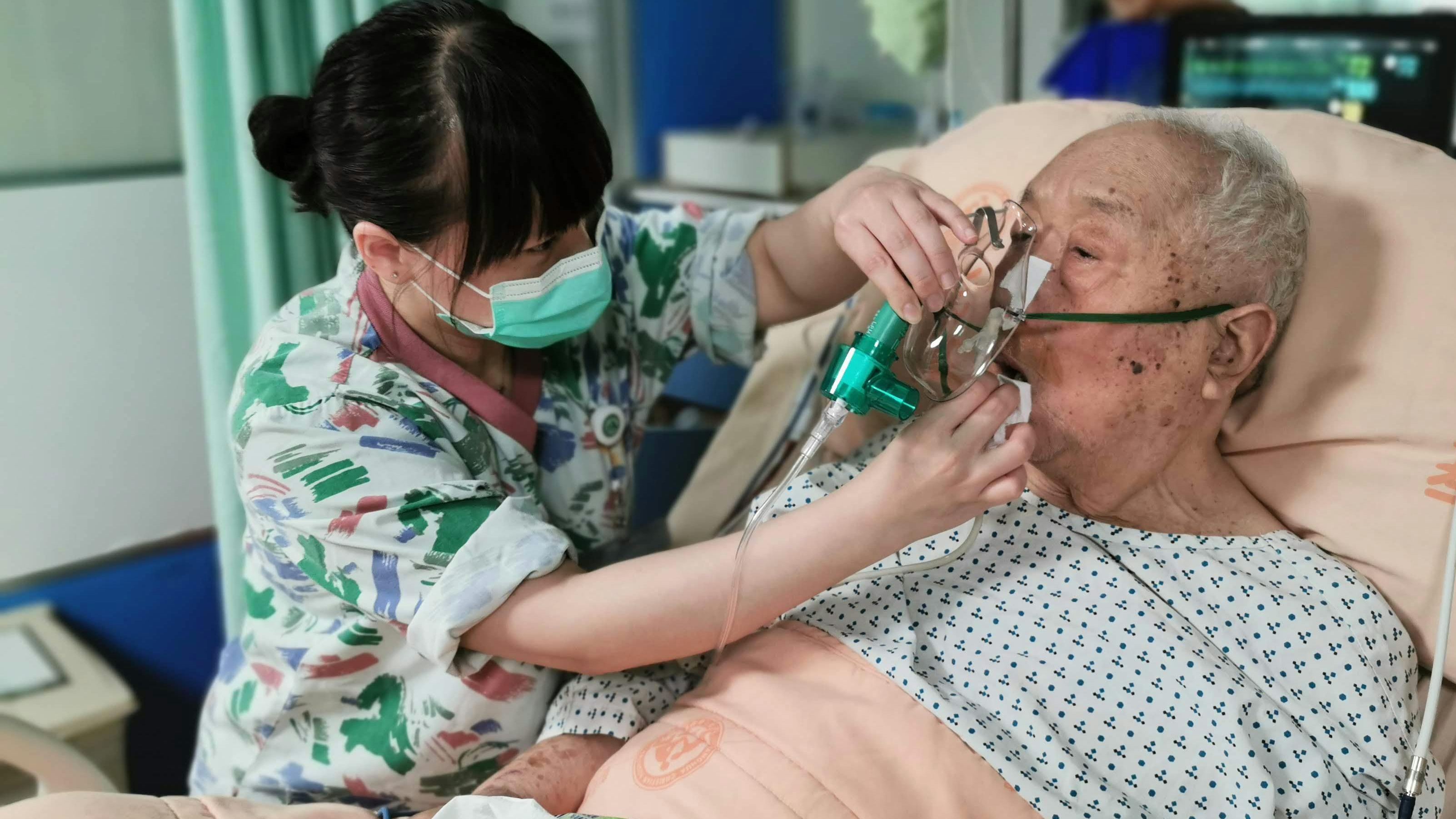
If you’ve ever filled out an advance healthcare directive, or helped your parent with one, you’ve likely come across the question of mechanical ventilation.
And if you’re like most people, you probably paused.
Because this isn’t just a medical checkbox. It’s a deeply personal decision that most people don’t fully understand until they’re forced to make it in a hospital, often under pressure.
While I'm not a physician, after over 30 years working in hospitals and long-term care, I can tell you this.
I was often the one sitting with families in those exact moments, helping them understand what mechanical ventilation really means and what their decision could lead to.
And too often, those decisions were made too quickly, without full clarity.
Let’s change that.
What Is Mechanical Ventilation?
Mechanical ventilation, often called “being on a ventilator” or “a breathing machine,” is a form of life support that helps a person breathe when they cannot breathe on their own.
A machine pushes air into the lungs through a tube, usually inserted through the mouth and into the throat, a process called intubation.
If ventilation is needed longer-term, a surgical opening in the neck, called a tracheostomy, may be created to make breathing more stable and comfortable.
In many cases, patients are sedated because the experience can be uncomfortable.
This is not a small intervention. It is full life support.
When a Ventilator Can Help
Mechanical ventilation can be incredibly beneficial in the right situations.
For example:
- During surgery
- After a sudden illness or injury
- When someone has a reversible condition like pneumonia or asthma
In these cases, the ventilator acts as a temporary support system, buying time for the body to heal.
People who tend to benefit the most are:
- Those who were relatively healthy before the illness
- Those expected to recover within days or weeks
- Those strong enough to come off the machine
In these situations, a ventilator can truly be life-saving.
When a Ventilator May Not Help as Much
This is the part many families are not prepared for.
Mechanical ventilation does not cure underlying diseases.
So if someone has:
- Advanced cancer
- Late-stage Alzheimer’s disease
- Severe heart, lung, liver, or kidney failure
The ventilator may prolong life, but it may not improve the overall condition or quality of life.
Additionally, people who are very frail or medically complex often have a much harder time coming off the ventilator.
The Risks and Realities of Long-Term Ventilation
Ventilators can help, but they can also create complications.
Some of the risks include:
- Increased chance of lung infections
- Weakening of breathing muscles over time
- Difficulty ever getting off the machine
- Inability to speak or swallow normally
In long-term cases, this can lead to:
- Feeding tubes
- Long-term placement in a care facility
- Skin breakdown or wounds from immobility
- Muscle contractures from being bedridden
These are not always discussed upfront, but they matter when making a decision.
Who Might Choose Mechanical Ventilation?
Some people choose ventilation because:
- They have a high chance of recovery
- They want to extend life as long as possible
- They are okay with potential complications
Others may choose it even for long-term use if they feel their quality of life would still be acceptable, for example, some individuals with spinal cord injuries.
Who Might Choose Not To?
Others may decide against mechanical ventilation because they:
- Want to avoid prolonged hospitalization
- Do not want to live dependent on machines
- Prioritize comfort over life extension
- Do not want the risks associated with long-term life support
And this is where your values, or your parent’s values, become the most important factor.
A Critical Question Most People Don’t Ask
When I sat with families, I would often guide them to ask the doctor:
- What are the chances of returning to previous functioning?
- Would this be short-term or long-term?
- What would daily life actually look like on a ventilator?
- What happens if things don’t improve?
Because here’s something many people don’t realize.
You can choose to try a ventilator, and later decide to stop it.
And ethically and legally, stopping a ventilator is not considered euthanasia. It is allowing natural death when treatment is no longer aligned with the person’s wishes.
The Emotional Side No One Talks About
This is where things get heavy.
Because the hardest part is not always the medical decision.
It’s the emotional weight of not knowing what your parent would have wanted.
I’ve seen families carry that burden for years.
And I’ve also seen families feel a deep sense of peace, simply because they had the conversation ahead of time.
Even if the decision itself was difficult.
Why Advance Care Planning Matters So Much
This is why conversations about things like mechanical ventilation matter before a crisis.
When preferences are discussed, or even written down, it becomes much easier to honor them when it counts.
If you haven’t already, this is where starting something like an advance healthcare directive for aging parents can make a huge difference.
And if you’re navigating these conversations now, you may also want to explore how to talk to your aging parent about medical decisions in a way that builds trust instead of resistance.
Final Thoughts
There is no “right” or “wrong” decision when it comes to mechanical ventilation.
There is only:
- What is medically possible
- What is realistically expected
- And what aligns with the person’s values
The goal is not to make the perfect decision.
The goal is to make an informed one.


